Oh, no. You just slipped on the icy sidewalk and now you have sharp back pain. Lots of questions may pop into your head. Did you slip a disc? Will this get better? Will you need surgery?
Don’t panic just yet. Although most of us don’t think about our vertebral discs until one of them starts to hurt, most (85%) improve in 8-12 weeks. Before we get into the treatment options, let’s start with the facts first: what are discs, and how can they be injured?
Discs are the cushions between almost all of your vertebrae (the separate pieces of your spine). Your spinal discs provide shock absorption, flexibility, and it prevents the bones from rubbing together (hooray for less friction).
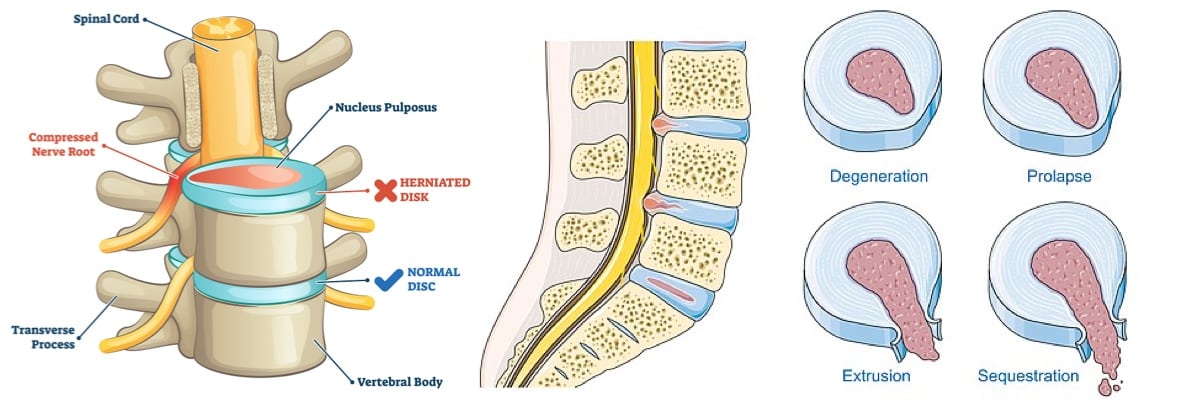
The vertebral disc is made of two parts: the annulus fibrosus (the tough outer layers) and the nucleus pulposus (the inner core of the disc, made of jelly-like material). Like a not-so-tasty cross of an onion and jelly donut.
There are a few things that can happen to your discs, and, while none of them are ideal, they do vary in pain level and severity.
This happens when the inner layer pushes on the outer layers of the disc, and the disc bulges all the way around–as if someone stepped on the middle of your peanut butter and jelly sandwich, and everything squeezed out. As terrible as it sounds, it’s not likely to cause many symptoms–and if it does, the symptoms are typically mild.
The outer layer of the disc tears, but the inner layer stays inside the disc. The patient may be asymptomatic or symptomatic. If symptomatic, the patient will feel pain at either the site of the injury, or they’ll have pain radiating down the arms from a disc tear in the neck, or down the legs from a tear in the low back.
This occurs when the outer layers of the disc tear or fissure, and the inner gel center oozes out. These types of disc injuries are much more likely to be symptomatic and the cases can vary from mild to severe. There are different types of disc herniation also:
Disc injuries can happen to nearly anyone, but there are specific groups that are more likely to get disc injuries than others. If you fit the bill for any or some of the following, you’ll be at a higher risk:
Typically, the lumbar spine or low back is the most common area for disc injury, especially the lower lumbar spine. Your cervical spine or neck is the second body area that is prone to disc injury. As much as most people don’t want to hear it, the combination of age and degeneration is the most common factor that causes the annulus to become more brittle and weak. As we age, our discs naturally become less hydrated, which makes them more dried out and less plump. The dried-out tough outer layers of a disc become more vulnerable to tearing, which can lead to a disc injury.
Repetitive body motions like lifting, twisting, and bending are the most common causes of shearing (or wearing down) stress placed on the disc. Disc injury can also result from sudden movements such as whiplash from a car accident.
Symptoms of disc injury can range from no symptoms, very little pain to debilitating pain and neurologic symptoms. Your chiropractor has extensive expertise in spinal and disc injuries and is best equipped to help to determine if you have a disc injury. Some clues that may lead you to suspect that you have a disc injury may include the following:
Now that you know what discs are, how they can be injured, who is at risk for injury, and how to determine whether you have a disc injury, you’ll likely want to determine how disc injuries are diagnosed and your treatment options. Check out the second part of this blog to find out more about the next steps with your healthcare provider, and how long it may take to heal from different treatment options.
Copyright @2025 Element Chiropractic — 875 SW Rimrock Way Suite 103, Redmond, OR 97756